- IHC Training
- Continuing Education Workshops
- Train the Trainer
- Veterinary Healthcare Communication
- Veterinary Communication Modules
- Online Learning for Continuing Education Credit
- Other Programs and Services
- Professional Development and Coaching
- Accreditation for CME/NCPD
- Evaluation & Research
- Licensing Materials
Train-the-Trainer Courses
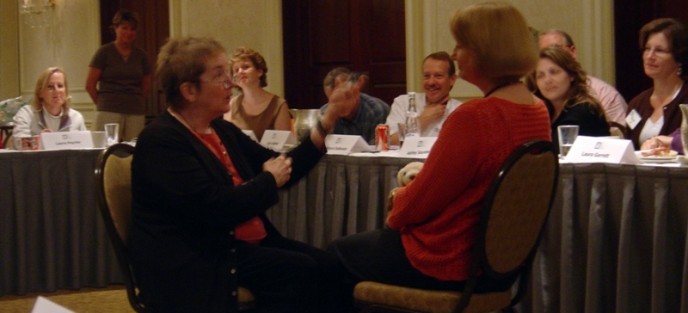
IHC’s “train-the-trainer” model enables widespread dissemination of IHC’s communication skills training. More than 3,000 healthcare team members have been trained as IHC faculty, conducting more than 500 workshops annually. IHC offers corresponding train-the-trainer faculty development courses for most IHC workshops to train faculty to conduct workshops at their home organizations. (Click here for IHC’s 2023 training calendar).
All of IHC’s faculty development courses are predicated on best practices in adult learning and clinician-patient communication. Active learning is encouraged through case-based discussions, large and small group exercises, video cases, and skills practice sessions. Most faculty development courses include skills practice with simulated patients (actors trained to portray patients, family members, or providers, and to provide feedback to learners). Course participants also practice presenting and facilitating various segments of the workshop they are studying. Under the direction of a trained course facilitator, they give feedback and provide coaching to one another as part of small group activities.
Participants in IHC train-the-trainer programs report high levels of achievement of the overall training goals:
- Learn workshop content, rationale and techniques, and gain confidence in workshop facilitation through practice
- Enhance their communication skills through small group exercises that may include simulated patients
- Explore and practice feedback and coaching skills
Train-the-trainer faculty development courses vary in duration, depending on the complexity of the subject matter. Faculty development courses are typically taught over three to five consecutive days.
IHC faculty development courses are designed for groups of 4 to 25 participants. The ratio of facilitators to participants is maintained at 1:4 or 1:5, depending on the topic. Continuing education credit is available to qualified participants who complete a faculty development course.
The process for becoming an IHC faculty member and conducting IHC workshops requires completion of an IHC faculty development course with practice assessment by an IHC Senior Trainer. Throughout each faculty development course, IHC Senior Trainers and small group facilitators provide feedback to learners and assess their readiness to conduct IHC workshops. In the event that additional support and coaching is needed prior to teaching an IHC workshop, IHC Senior Trainers are available to provide such personalized support and guidance. Individualized support is scheduled separately and subject to additional fees.
All IHC faculty must use the most up-to-date version of IHC’s copyrighted curricular materials for the course(s) they are trained to lead.
“IHC has contributed enormously to my ability to teach physicians one of the most important parts of the patient-provider relationship — solid, effective communication.” — James R. Gavin, III, M.D., Ph.D., Past President, Morehouse School of Medicine
IHC train-the-trainer faculty development courses employ an array of educational formats based on evidence cited in the literature. To maximize learning, a variety of teaching methodologies are used to account for differences in learning styles. Learning objectives include the acquisition of knowledge and concepts (cognitive), attitudes (affective), and practice opportunities (skills). The following table provides a summary of the educational formats used in IHC courses and rationales for each format.
IHC course formats and rationale
Educational Formats Rationale Didactic Conveys course content, concepts, principles and relevant research. Discussion Provides a forum for presenting and sharing ideas, feedback, and responses to questions while demonstrating understanding of CME activity content and concepts. Case study Provides learners with value of seeing health care situations in context and “though patients’ eyes” and opportunity to analyze and assess the quality and impact of a clinician-patient interaction. Experiential exercise Maximizes the assimilation and reinforcement of course content and concepts through “hands-on” activities. Simulation Applies targeted communication skills and problem-solving strategies to planned interactions with patients and colleagues. Differentiated from role-playing, simulations involve professional actors to portray clinician interactions with patients and/or colleagues. Audio-visual – Training film Provides learners with opportunity to view case studies to identify effective and ineffective communication techniques and approaches, respond, share reactions to film content and discussion points. Role-play Provides simulation exercises for the purpose of applying newly learned skills and opportunities for learners to appreciate patient and clinician experience. Planned interactions are presented by the learners, in contrast to professional actors (see Simulation). Reflection Encourages the learner to ask more questions, invite deeper consideration of an issue/question, and provides a supportive forum for exploration of one’s values, beliefs and attitudes that impact healthcare interactions. Pair share Allows learners to work with a colleague to examine a problem, discussion topic or task, and provide mutual feedback. Small group presentation Provides forum for exchanging thoughts, opinions, skills and reaching consensus. Small group exercise Strengthens learners’ ability to retain information through social interaction involved with cooperative learning within socially appropriate norms.
IHC can customize faculty development training options to accommodate organizations’ particular needs. For example, faculty development courses on disclosure are customized to reflect policies, procedures and special considerations of individual provider organizations, states and levels of care. We can also accommodate requests to include added time with simulated patients. For information about IHC faculty development courses for your organization, please contact info@healthcarecomm.org.
Click here to view our 2023 calendar of training events.